
In October 2023, Robert got a preview of medical troubles that awaited him—in 2024, he had five hospital admissions and three ER visits for infections and difficulty breathing. It began with a 3:00 a.m. 911 call that led to a week-long hospital stay featuring his three kidney conditions: absence of a right kidney, multiple cysts causing Acute Kidney Injury, and severe (stage IV) Chronic Kidney Disease.
Prayer was central to navigating Robert’s care. I prayed to the Lord. Church prayer warriors prayed. Family and friends prayed. We all trusted God to give us wisdom for decisions to be made, qualified medical personnel, and provision for his every need.
Want to subscribe to receive blog updates sign up today!
“. . . for we do not know what to pray for as we should, but the Spirit Himself intercedes for us with groanings too deep for words; . . . He intercedes for the saints according to the will of God.” Romans 8:26-27 (New American Standard Bible).
And God was faithful. In answer to our prayers, Robert’s medical needs were met without dialysis. On October 13, 2023, he was discharged to home with oxygen, medication, and home health. Sadly the reprieve was only temporary.
Twenty weeks later, Robert was once again in the ER fighting for his life. His kidney function had virtually stopped and had reached Stage V, End Stage Renal Disease. In response to many prayers, God brought Robert back from the brink of death. However, this time hemodialysis was needed to remove blood from his body, send it to the hemodialysis machine for cleansing, and return the clean blood back into his body.
Dialysis treatment began in the hospital, continued in an acute rehabilitation hospital, and carried over to an outpatient center. However, the transition from inpatient to outpatient dialysis was fraught with frustration. Prayers were needed to overcome the angst caused by the case manager at the rehabilitation hospital. First she dragged her feet in notifying the local dialysis center of Robert’s imminent need for chair time; then she referred me to dialysis centers in neighboring counties saying there was no chair time available in our town. This meant I would have to wait for him at the center three and a half hours instead of returning home during his treatment.
But God took care of the situation. Right when I was at the end of my rope, the Nurse Practitioner from Robert’s kidney doctor’s office appeared. After I told her what was happening, chair time miraculously became available five miles from home!
Before beginning outpatient dialysis, I met with the center manager to discuss the accommodations Robert would need. Given his inability to independently get on and off the dialysis chair, she promoted Robert’s switch to at-home dialysis.
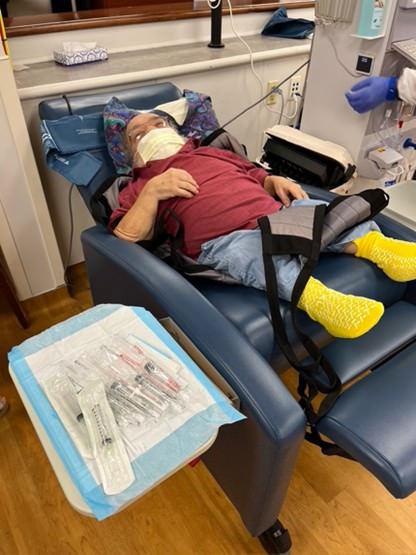
My instinct told me the manager preferred for Robert to be treated elsewhere. Nonetheless, I politely listened to the pitch for Peritoneal Dialysis (PD)—a needle-free at home treatment where waste is filtered from the blood via a solution input into the abdomen using the peritoneal lining. In contrast, hemodialysis uses two needles.
Whatever the manager’s motivation, Robert’s kidney doctor directed that he begin treatment with in-center hemodialysis. She approved using a Hoya lift to get Robert onto the dialysis chair, but disapproved staff stepping outside the building to help him get to and from the van into the center. Initially Robert was able to safely ride his scooter independently up and down the van ramp and across the parking lot to the entrance. However, as his cognitive acuity and physicality declined so did his ability to drive his scooter. How was I going to get him into the center? I couldn’t manually push Robert up and down the ramp in a wheelchair or scooter. This is when God reminded me of a past practice we had of riding the scooter tandem when we only brought one scooter to an event—we raised the scooter tiller to vertical, one of us sat, and the other stood on the scooter platform and drove. So this is what we did. Plus we moved the dialysis bag to hang off the armrest. Problem solved.

For eight and a half months, Robert and I trekked three times a week to the outpatient dialysis center. He typically emerged from sessions complaining of refrigerator like temperatures, headaches, various aches and pains, and exhaustion. Yet one thing was still intact. His appetite. So we quickly developed two takeout traditions on our way home—Taco Tuesday was a buy one get one free (BOGO) deal and Dunkin Donuts beckoned us on Thursdays despite lacking a BOGO lure. (Believe it not, neither of these treats were renal diet cheats!) Saturdays were open for spontaneity.
Long after the 90-day timeline for the dialysis tunneled catheter in the vein below Robert’s right shoulder had expired, Robert was referred to two surgeons in search of alternatives with less infection risk and minimal needle trauma. However, after evaluating Robert for creation of a dialysis fistula—connecting an artery and a vein—the vascular surgeon rejected him as a candidate for this procedure given his short arms and peripheral artery disease in his legs. A second surgeon approved Robert for a peritoneal catheter placement. However, one week before the scheduled surgery, Robert was admitted to the hospital with sepsis and never recovered sufficiently for the surgery to be rescheduled.
A kidney transplant may have been the ultimate solution to Robert’s vein access issues, but an information appointment was cancelled due to his ER visit for falling out of bed. Likewise subsequent admissions to hospital and rehabilitation facilities squelched further exploration of a kidney transplant.
Hospitalizations were initiated by the dialysis center when Robert passed out during a treatment in October with shortness of breath and a COVID infection in November. In December, two more respiratory episodes led to ER visits. The differential diagnosis lists added “worsening renal failure” and “congestive heart failure” exacerbation.
On December 11, 2024 Robert went to a make-up dialysis session after missing his regularly scheduled treatment the day before. He was miserable. The dialysis social worker could see this and called me to report her conversation with Robert. Knowing his expressive communication was limited, she elicited his responses with a caring comment followed by two questions:
- “I hate to see you suffering like this Robert, do you want to continue dialysis? He answered with a decisive “no.”
- “Do you know what happens if you stop dialysis?” Robert replied, “I will die.”
I did not anticipate Robert’s dialysis ending this way. Nonetheless as his Health Care Surrogate, I honored his choice and thanked God that Robert saved me from having to make the decision for him. God knew how much we could handle and saw we were both close to breaking point.
But He knows the way I take;
When He has put me to the test, I will come out as gold.
My foot has held on to His path;
I have kept His way and not turned aside.
Job 23:10-11 (New American Standard Bible)
You may also want to read:
- Angela Muir Van Etten. Institutional Care. June 4, 2025. https://angelamuirvanetten.com/institutional-care/
- Treatment Options for Kidney Disease. Fresenius Kidney Care. https://freseniuskidneycare.com/treatment
- Treatment Options for End Stage Kidney Disease. Davita Kidney Care. https://www.davita.com/treatment-options/
- Dialysis Fistula. Cleveland Clinic.
https://my.clevelandclinic.org/health/procedures/dialysis-fistula - Peritoneal Dialysis. Cleveland Clinic.
https://my.clevelandclinic.org/health/procedures/peritoneal-dialysis
