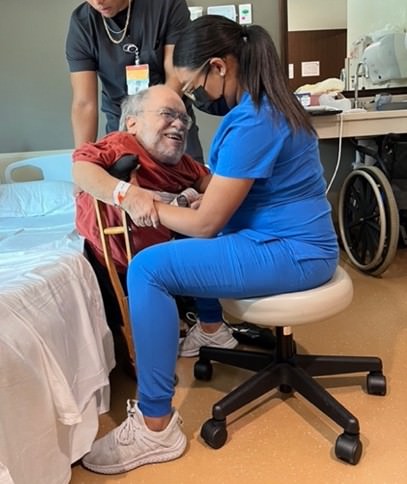
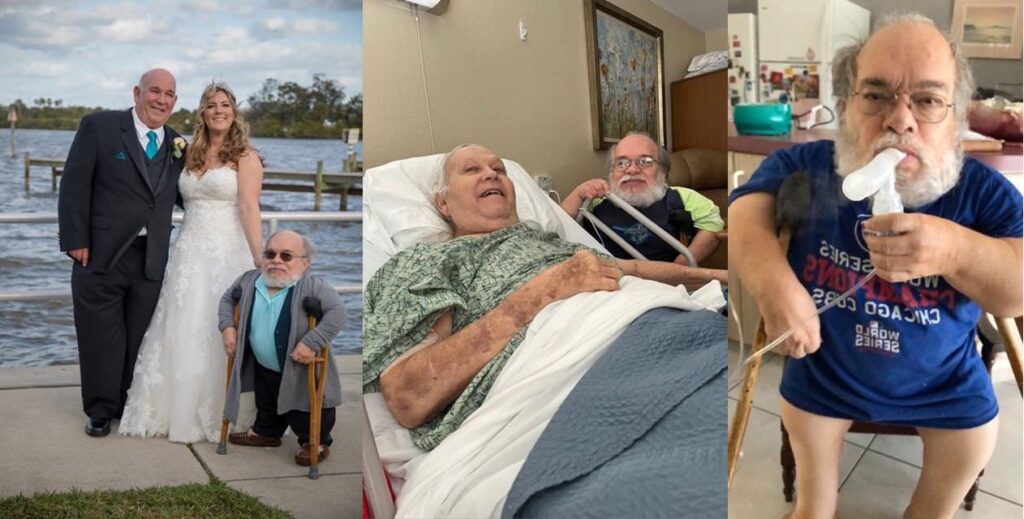
My life changed forever the day I met Robert. Our love for one another motivated me to change—my country, my church, my job—everything. Likewise everything changed the day Robert died. But this time the change was out of my control and it was the end of our marriage not a beautiful beginning. Bridal bliss was replaced with a widow’s sorrow. There would be no more of his adventures, caring, encouragement, hugs, laughter, love, smiles, or stories—no more anything with him.
Although it seemed like my world stopped, I was caught up in a flurry of activity with family and friends involving cremation, a celebration of life service, and the first round of distributing, donating and tossing Robert’s worldly goods. Despite the sadness, family helped nourish my body at favorite restaurants and my spirits at a butterfly park and art museum.
Want to subscribe to receive blog updates sign up today!
And as expected, after a few weeks everyone returned to their own routines. I was okay with this. Because Robert had been in residential rehabilitation or hospital care for several months before he died, I was used to living alone. So I went about my days taking care of what was in front of me—paying bills, medical appointments, online groceries, teaching Sunday School, et al. However, I felt flat, frittered away a lot of time watching TV, and lacked the creativity and concentration needed for anything extra. Clearly the mere passage of time was not enough for me to fully recover from losing Robert.
I needed a healthy way to mourn my loss. GriefShare—a 13-week support group that has helped more than one million people find comfort as they move through the grief process—is how I’m paving my path forward. Through a Bible-based work book, videos, and group discussions I’m learning six important processes to work through in order to heal the pain. As I approach the one year anniversary of Robert’s death, it’s a good time to pause and reflect on six signs of healing—accepting, adjusting, dealing with emotions, continuing, sharing comfort, and addressing questions. (GriefShare®, p ix, fourth edition, April 2024.)
Accepting that I won’t see Robert again on this earth is a given; rather I’m acknowledging that every aspect of my life is changing. I can’t go on as though nothing has happened. And numbing the pain with escape behaviors keeps me stuck in grief. Instead, adjusting to being a widow calls me to embrace a different role in society. So I’m reassessing how God wants me to use my gifts, talents, and skills and staying open to any changes God wants me to make.
The first focus was my blog begun five years earlier as a tool for marketing my dwarfism memoir trilogy. I asked God whether to discontinue or remodel the blog. After a five month pause, the answer was apparent. Restart the blog and reduce the frequency to once a month.
My biggest challenge to adjusting has been with household maintenance issues. I was bombarded with opportunities to adjust when the pool pump got so loud it disturbed the neighbors, brown patches appeared in the lawn after the sprinkler clock quit, the air conditioner failed to keep the house temperature comfortable, water cascaded off the roof when the gutters clogged, a leaking pipe on the solar panel dripped onto the patio, and termites were discovered in the attic. Dealing with contractors had been Robert’s department. Now it was my job to get bids from reputable businesses, understand the equipment, and negotiate the scope of the work and fair prices. I hated the process, but trusted God to lead me to competent and reliable workers.
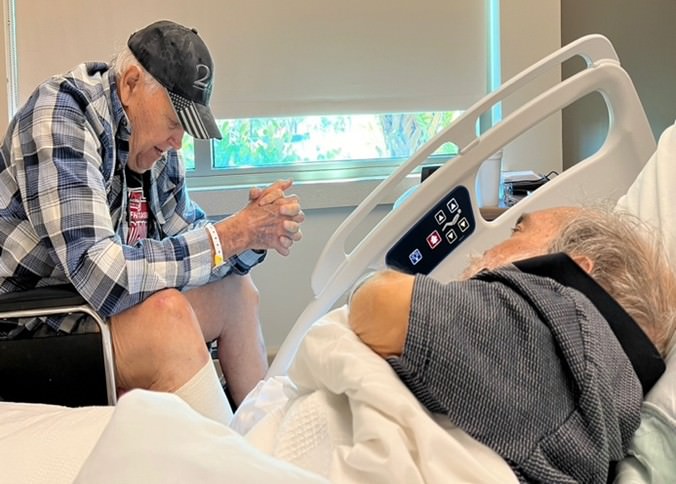
Relationships also required adjusting. Despite the high value I place on being independent, the large volume of maintenance issues caused me to rely on help from family, friends, and neighbors. Breaking two fingers and being in a hand splint for six weeks saw many of these same helpers provide meals and drive me to appointments, church, and other events. The bonus was that our bonds grew stronger as we spent more time together. My relationship with Robert’s brother Mickey and his daughter Veronica (his caregiver) also strengthened when I visited him regularly to provide stimulation and encouragement and give Veronica much needed breaks and emotional support.
Sadness is the primary emotion I deal with in my healing process. Rather than being angry and bitter that Robert’s gone, I thank God for our 43 years of marriage and for ending his suffering. I alleviate my sadness with music and memories. Remembering him with photos, in conversations, and on special days helps fill the void. On his birthday, I celebrated with family at the same place Robert ate with us last year. On our wedding anniversary, I ate a slice of cheesecake remembering how much he enjoyed this treat last year while in a rehabilitation facility. Naturally I also remember him on ordinary days!
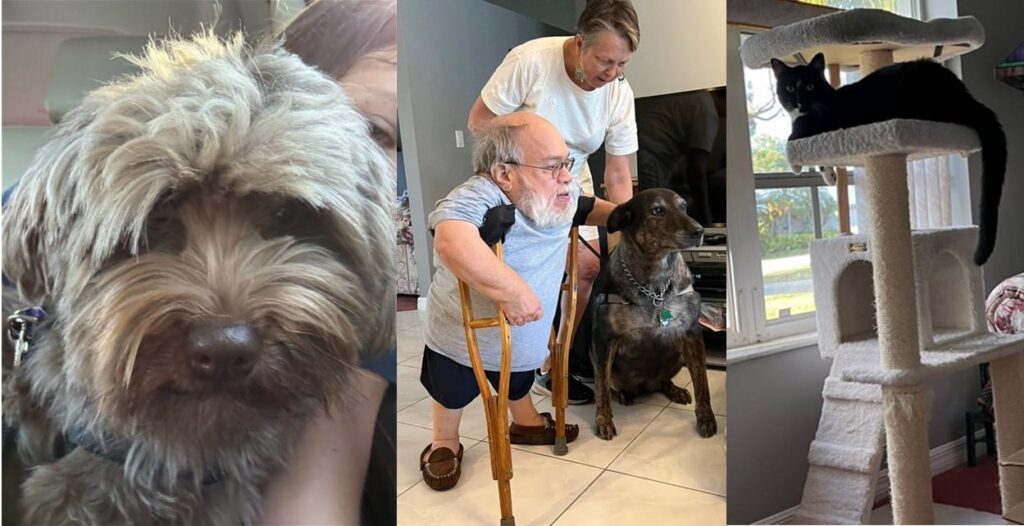
In continuing life without Robert I take steps forward in a way that honors his memory. For example, I provided biographical material to Robert’s professional organization—the Rehabilitation Engineering Society of North America (RESNA)—in support of his posthumous Fellow Award; gave Robert’s close friends and family a photo magnet of him enjoying six of God’s creatures; and continued our Christmas tradition of shopping in charity gift catalogues as an alternative to buying presents for each other.
I don’t try to replicate the way things were, but I have continued our practice of hospitality. Two of these events Robert used to enjoy—our Little People of America chapter Thanksgiving party and family reunions. He was not here for this year’s baby shower or welcome dinner with our new Pastor’s family and church friends.
“Comforting others is essential to your healing.” (GriefShare®, p ix, fourth edition, April 2024.) I found my comfort in God, “our merciful Father and the source of all comfort. He comforts us in all our troubles so that we can comfort others. When they are troubled, we will be able to give them the same comfort God has given us.” (2 Corinthians 1:3-4, New Living Translation.) Because I was very aware of how important it is to have family at your side in the aftermath of a loved one’s death, I comforted a grieving mother by contributing to the travel expenses of her siblings who lived thousands of miles away.
“A key step toward healing involves coming to terms with what you believe about God, heaven, and eternity.” (GriefShare®, p 101, fourth edition, April 2024.) This was an easy one for me. My views on such matters were settled long before Robert’s death. We both believe that Jesus is our Lord and Savior, Robert is alive in Christ, and we’ll be reunited when I die or Jesus returns, whichever comes first. The day is coming when “[God] will wipe every tear from their eyes, and there will be no more death or sorrow or crying or pain. All these things are gone forever.” (Revelation 21:4, New Living Translation)
Meanwhile, I’m trusting God’s plan and goodness. Based on His faithfulness to me in the past, I’m confident He will keep His promises in the future. I can be sure of this, “God is with [me] always even to the end of the age.” (Matthew 28:20)
For further information on GriefShare, go to: https://www.griefshare.org
For more Angela Muir Van Etten blog posts in the series Until Death Us Do Part, go to:
- More Valuable Than Sparrows. November 5, 2025. https://angelamuirvanetten.com/more-valuable-than-sparrows/
- Physical Therapy Journey. October 1, 2125. https://angelamuirvanetten.com/physical-therapy-journey/
- Caregiving with Help. September 3, 2025. https://angelamuirvanetten.com/caregiving-with-help/
- Caregiving at Home with Love and Faith. August 6, 2025. https://angelamuirvanetten.com/caregiving-at-home-with-love-and-faith/
- Dialysis Prayer Walk. July 2, 2025. https://angelamuirvanetten.com/dialysis-prayer-walk/
- Institutional Care. June 4, 2025. https://angelamuirvanetten.com/institutional-care/
For Angela and Robert Van Etten’s love story, read “Pass Me Your Shoes: A Couple with Dwarfism Navigate Life’s Detours with Love and Faith” by Angela Muir Van Etten. https://www.amazon.com/Pass-Me-Your-Shoes-Navigates/dp/0998464864/ref=sr_1_1?dchild=1&keywords=pass%20me%20your%20shoes&qid=1600969039&s=books&sr=1-1&fbclid=IwAR2SO81IzPfczzW2MPyCHKRHvoQTQDulyzwywq2G_fgpIMyaQCV1zkIQFJo
For Scripture supporting my belief that Robert is alive in Christ and that we will be reunited when I die, go to: Luke 24; John 14:1-3; Romans 1:16-17, 3:23-25, 5:8-10, 6:4-11, 23, 8:1-4, 11, 31-34, 10:9-10, 13; 1 Corinthians 15:22, 35-58; Philippians 3:20-21; and 1 Thessalonians 4:14.